Diabetic Foot
WHAT IS DIABETIC FOOT?
Diabetic foot refers to a range of foot problems that can occur in individuals with diabetes. High blood sugar levels over time can lead to nerve damage (neuropathy) and poor blood flow (peripheral arterial disease) in the feet. This combination can make the feet more susceptible to injury and slow to heal.
What are signs of diabetic feet?
Dry, cracked skin on your feet. A change in the color and temperature of your feet. Thickened, yellow toenails. Fungus infections such as athlete’s foot between your toes.
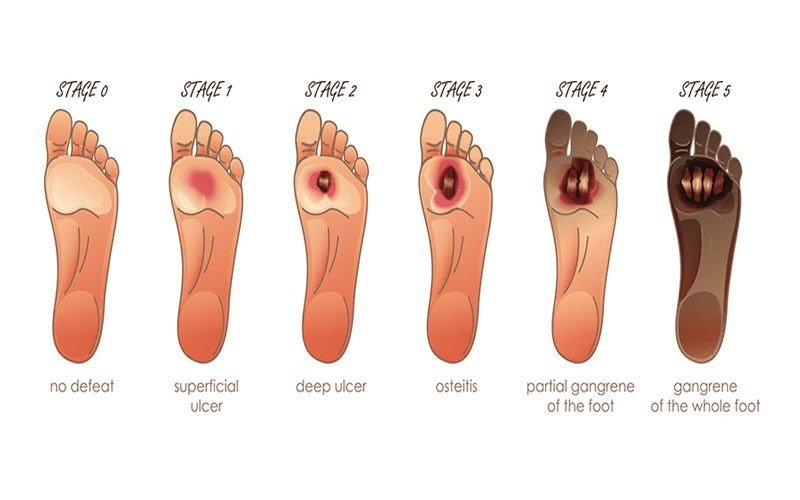

Is diabetic foot is serious?
The infection may not heal well because the damaged blood vessels can cause poor blood flow in your feet. Having an infection and poor blood flow can lead to gangrene. That means the muscle, skin, and other tissues start to die.
What foods are bad for diabetics?
Full-Fat Dairy: Full-fat dairy products include rich cheese, cream, and whole milk.
Trans Fat: Trans fat is another food to avoid if you have diabetes.
White Carbohydrates
Fried Foods
Alcohol
Processed Meats
High-Fat Cuts of Meat
Packaged Cookies and Pastries


Is Diabetic foot is curable ?
Diabetic foot, a complication of diabetes, can be managed and treated, but it is not always curable in the traditional sense. The key to managing diabetic foot is through a combination of lifestyle changes, proper foot care, medication, and, in some cases, surgery.
To prevent diabetic foot complications, it’s essential for individuals with diabetes to maintain healthy blood sugar levels, manage their weight, exercise regularly, and inspect their feet daily for any signs of problems. It’s also crucial to wear proper footwear and to seek prompt medical attention if any issues arise.
While diabetic foot complications can be challenging to treat, especially in advanced cases, early detection and proper management can significantly improve outcomes and quality of life.










